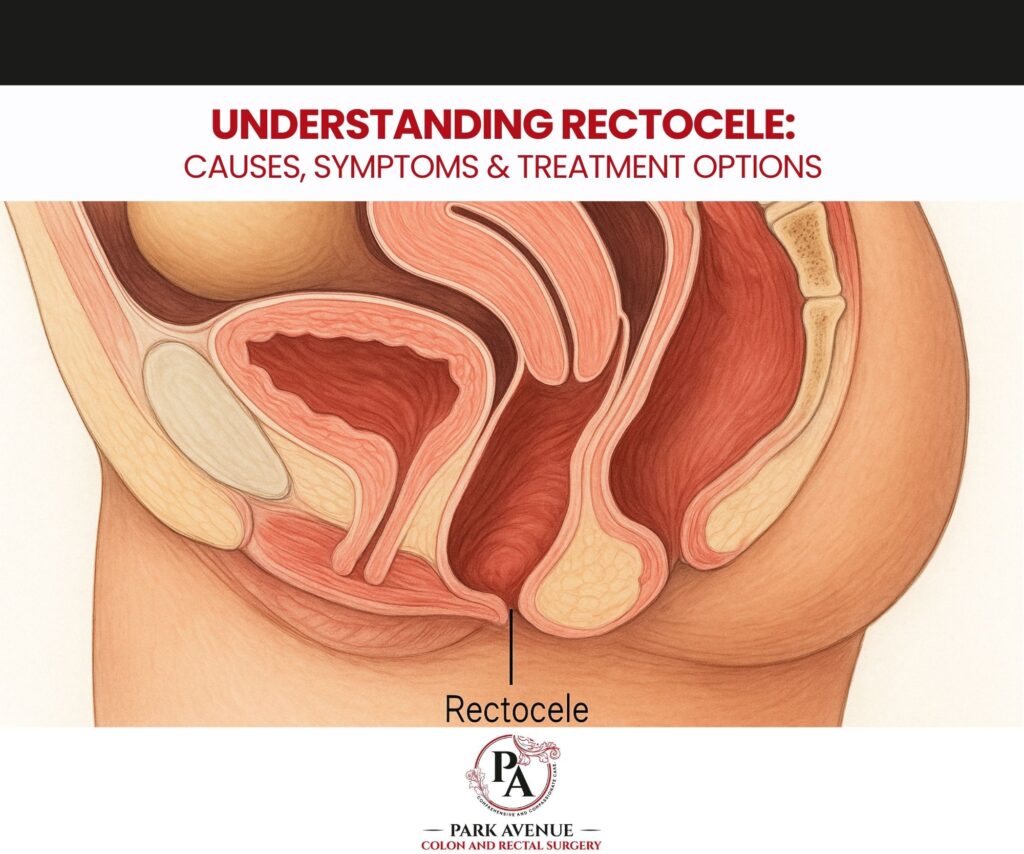
A rectocele—sometimes called a posterior vaginal prolapse—occurs when the rectal wall bulges into the vaginal wall due to weakened pelvic floor support. While common, especially among women who have given birth, rectocele is often underdiagnosed because many patients hesitate to discuss pelvic symptoms.
At Park Avenue Colon and Rectal Surgery, we believe in compassionate, comprehensive care that empowers patients with clear information and evidence-based treatment options. Below, we explore what a rectocele is, why it happens, and how it can be treated effectively.
What Is a Rectocele?
A rectocele develops when the supportive tissues between the rectum and vagina stretch or weaken, allowing part of the rectum to protrude into the vaginal canal. Depending on its severity, a rectocele can be mild and asymptomatic—or significant enough to interfere with bowel movements and daily comfort.
Rectoceles often occur alongside other pelvic floor disorders such as cystocele (bladder prolapse) or uterine prolapse, but they can also occur on their own.
Common Causes of Rectocele
Rectoceles can develop from a combination of factors that weaken pelvic support structures over time, including:
- Childbirth trauma, especially with large babies, forceps delivery, or prolonged pushing
- Chronic constipation or straining during bowel movements
- Aging and menopause, when hormonal changes reduce tissue elasticity
- Prior pelvic or rectal surgery
- Heavy lifting or chronic coughing
- Genetic predisposition affecting collagen or connective tissues
Understanding the underlying cause helps guide treatment and prevention strategies.
Symptoms of Rectocele
Some people with rectocele experience no symptoms, especially in mild cases. Others may report:
- A sensation of pelvic pressure or bulging
- Difficulty emptying the bowels
- The need to apply pressure inside the vagina to complete a bowel movement (splinting)
- Chronic constipation
- Pain or discomfort during intercourse
- A visible bulge in the vaginal opening in more advanced cases
If these symptoms are affecting your quality of life, evaluation by a specialist is recommended.
How Rectocele Is Diagnosed
At Park Avenue Colon and Rectal Surgery, diagnosis is conducted with expertise and sensitivity. Evaluation may include:
- Detailed medical history and symptom review
- Physical and pelvic examination
- Defecography or pelvic imaging, if needed, to assess severity and additional pelvic floor issues
Accurate diagnosis ensures the most effective and personalized treatment plan.
Treatment Options for Rectocele
Treatment depends on the severity of symptoms and your overall health. Options may include:
1. Non-Surgical Management
- Pelvic floor physical therapy
- Dietary changes to reduce constipation
- Stool softeners or fiber supplementation
- Avoiding heavy lifting and straining
- Pessary device, which supports the vaginal wall and reduces bulging
These approaches are often effective for mild to moderate rectoceles.
2. Surgical Repair (Rectocele Repair)
Surgery may be recommended when symptoms significantly affect daily activities or conservative treatments are unsuccessful. Surgical goals include:
- Reinforcing or reconstructing weakened tissues
- Reducing bulging
- Restoring bowel function and pelvic support
Modern techniques allow for faster recovery, excellent results, and improved quality of life.
Rectocele Frequently Asked Questions (Q&A)
1. Is rectocele dangerous?
Rectocele is usually not life-threatening, but it can significantly impact comfort and bowel function. Early evaluation prevents worsening symptoms and helps identify the best treatment strategy.
2. Can rectocele heal on its own?
Mild rectoceles may improve with pelvic floor therapy and lifestyle modifications, but moderate to severe cases typically require medical or surgical intervention.
3. What happens if a rectocele is left untreated?
Symptoms may gradually worsen, leading to increased difficulty with bowel movements, discomfort, pelvic pressure, and decreased quality of life.
4. Does childbirth always cause rectocele?
Not always. While childbirth increases risk, many women never develop rectocele, and some who have never given birth can still experience it due to other factors.
5. What can I do to prevent rectocele?
- Maintain a high-fiber diet
- Avoid straining and treat constipation early
- Perform regular pelvic floor exercises
- Avoid heavy lifting
- Seek evaluation for chronic coughing or pelvic pain
6. How long is recovery after rectocele surgery?
Recovery varies, but most patients resume normal activities within a few weeks. Heavy lifting and strenuous exercise are typically avoided for 6–8 weeks.
7. When should I see a specialist?
If you experience persistent pelvic pressure, bowel difficulties, or vaginal bulging, a specialist evaluation ensures timely and effective care.
Expert Care at Park Avenue Colon and Rectal Surgery
Rectocele can be a sensitive topic—but you don’t have to navigate it alone. Our practice provides thoughtful, specialized care to help patients regain comfort, function, and confidence.
Contact Information
Park Avenue Colon and Rectal Surgery
📍 36 E 36th St, 1C, New York City, NY 10016
📞 Phone: (646) 822-0228
🌐 Website: marshaharrismd.com
🗓️ Appointments: https://marshaharrismd.com/appointments
