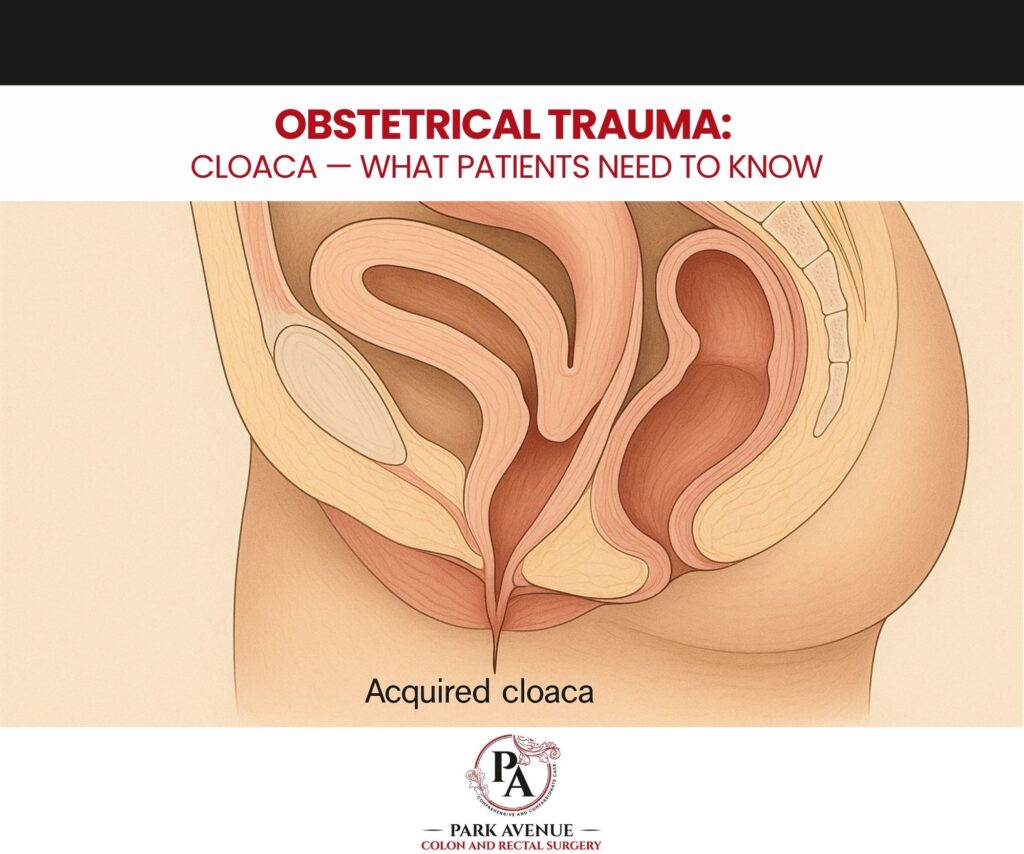
Obstetrical trauma can lead to a range of pelvic and perineal complications, but one of the most complex and challenging conditions is the development of a cloaca-like defect. While cloaca is typically a congenital anomaly, severe birth-related injury can result in acquired cloacal deformities, where the rectum, vagina, and urinary tract may become structurally compromised or confluent due to trauma.
At Park Avenue Colon and Rectal Surgery, we are committed to providing compassionate, expert care for women experiencing the physical and emotional impacts of obstetrical trauma. This post explains what an acquired cloaca is, why it occurs, how it is diagnosed, and the available treatment options.
What Is an Acquired Cloacal Deformity?
In adults, the term “acquired cloaca” refers to a complex pelvic floor and perineal breakdown in which structures such as the rectum, vagina, and urethra become interconnected due to traumatic injury. Unlike congenital cloaca, this condition is not present at birth—it occurs as a result of tissue damage and improper healing.
Common causes include:
- Severe obstetric lacerations from childbirth
- Prolonged labor or obstructed labor
- Instrument-assisted births (forceps or vacuum)
- Infection leading to tissue breakdown
- Incorrect or incomplete repair of earlier perineal tears
- Trauma-related fistula formation
When these structures lose their natural separation, patients may experience significant functional, cosmetic, and emotional consequences.
Symptoms and Impact
Women with cloacal-type injuries may experience:
- Fecal or gas incontinence
- Chronic pelvic pain
- Urinary leakage or difficulty voiding
- Painful intercourse
- Recurrent infections
- Abnormal openings or passage of stool through the vagina (rectovaginal fistula)
These symptoms can be distressing and may significantly affect quality of life. Fortunately, specialized colorectal surgical care offers effective treatment options.
Diagnosis: A Thorough, Sensitive Approach
Accurate diagnosis is essential due to the complexity of the pelvic structures involved. Evaluation may include:
- Detailed physical and pelvic examination
- Endoanal ultrasound
- MRI or CT imaging for soft-tissue visualization
- Specialized anorectal function testing
- Collaboration with urogynecology or pelvic floor specialists
At Park Avenue Colon and Rectal Surgery, diagnostic care is performed with utmost respect, privacy, and sensitivity.
Treatment Options
Treatment depends on severity, symptoms, and structural involvement. Options may include:
1. Surgical Reconstruction
Rebuilding pelvic anatomy often involves:
- Separation of fused structures
- Repair of sphincter injuries
- Correction of fistulas
- Restoring the natural alignment of the rectum, vagina, and urethra
2. Staged Surgical Approaches
Complex cases may require multiple surgeries for optimal results.
3. Pelvic Floor Rehabilitation
Therapy can help improve continence and functional outcomes.
4. Management of Associated Conditions
This may include addressing infections, scarring, or chronic inflammation.
With proper intervention, many patients regain function, comfort, and confidence.
Comprehensive Q&A: Obstetrical Trauma and Cloaca
Q: Is a cloaca always a congenital condition?
A: No. While congenital cloaca occurs in newborns, acquired cloacal deformities can develop in adults due to severe obstetrical trauma or tissue breakdown after childbirth.
Q: How common is this condition?
A: It is considered rare, but pelvic floor injuries during childbirth are not. Severe perineal tears occur in 3–6% of deliveries, and some poorly healed injuries can evolve into more complex deformities.
Q: What symptoms should prompt an evaluation?
A: Any unexpected passage of stool or gas from the vagina, persistent pelvic pain, difficulty controlling bowel movements, or abnormal anatomy should be evaluated by a colorectal surgeon.
Q: Can these injuries heal without surgery?
A: Minor tears can heal conservatively, but complex cloacal-type injuries generally require surgical reconstruction to restore normal anatomy and function.
Q: Who is the ideal specialist for treating this condition?
A: A colorectal surgeon with expertise in pelvic floor reconstruction, often working collaboratively with urogynecologists and pelvic health specialists, is best suited for managing this condition.
Q: What is recovery like?
A: Recovery varies by procedure. Many patients resume normal activities within weeks, with full healing over several months. Pelvic therapy may enhance long-term outcomes.
Q: Will treatment improve continence?
A: Many patients experience significant improvement in continence, comfort, and quality of life after reconstruction and rehabilitation.
Why Choose Park Avenue Colon and Rectal Surgery?
Our practice is dedicated to providing specialized care for complex colorectal and pelvic floor conditions. We prioritize:
- Expert surgical care
- Compassionate, patient-centered evaluations
- Clear communication and individualized treatment plans
- A comfortable, supportive environment
Your health and dignity are always our top priorities.
Contact Us
Park Avenue Colon and Rectal Surgery
📍 36 E 36th St, Suite 1C, New York City, NY 10016
📞 Phone: (646) 822-0228
🌐 Website: https://marshaharrismd.com
📅 Appointments: https://marshaharrismd.com/appointments
If you believe you are experiencing symptoms related to obstetrical trauma or an acquired cloacal injury, reach out today for a private, expert evaluation.
